When you have Corneal Arcus (Arcus Senilis) eye disorders, your eye doctor may perform additional tests to rule out other conditions and find the cause of your eye discomfort. But since arcus senilis is considered both normal and benign for the elderly, no treatment is required or recommended. If you have additional questions please come to Manhattan Pediatric Eye Doctors & Specialists, the best rated eye doctors in NYC. Meet your local optometry specialist Dr. Saba Khodadadian and the best in class opthamologist in NYC Dr. Daniel Khodadadian.
Corneal Arcus (Arcus Senilis)
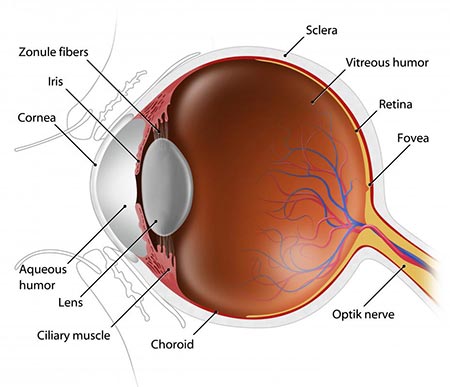 Corneal arcus generally appears in older people, which is why it’s also called arcus senilis. Arcus senilis is a circular ring in the periphery of your cornea made up of cholesterol deposits. A flaxen or gray-colored band forms, circling the cornea of each affected eye. This opaque halo surrounding your cornea’s stromal layer has a distinct border on the outside while the inside border is less defined.
Corneal arcus generally appears in older people, which is why it’s also called arcus senilis. Arcus senilis is a circular ring in the periphery of your cornea made up of cholesterol deposits. A flaxen or gray-colored band forms, circling the cornea of each affected eye. This opaque halo surrounding your cornea’s stromal layer has a distinct border on the outside while the inside border is less defined.
The material is made of an abnormally high level of phospholipids and cholesterol deposits. The phospholipid sediments of the corneal arcus generally start at the bottom and the top of your cornea. However, these deposits can eventually expand to completely cover the entire circumference of your cornea, which is usually when you start having vision problems.
At Greatest Risk
The condition affects about 60 percent of the population between 50 and 60 years old. For persons over the age of 80, corneal arcus afflicts nearly 100 percent of those tested. The incidence is even higher in the African American population, although researchers aren’t sure why.
When corneal arcus occurs in those less than 40 years old, the name used for the condition is arcus juvenilis. It’s usually associated with higher than normal lipid levels, generally consisting of esterified cholesterol in the blood — cholesterol that’s been chemically altered. This medical condition is often referred to as hypercholesterolemia.
The majority of people over the age of 70 or 80 develop gray or yellowish circular rings around the corneal periphery. Corneal arcus is more common in people of Asian and African origin as compared to Caucasians. Men are more likely than women to develop the age-related arcus senilis, and this difference increases incrementally with age. The yellowish ring also has a strong correlation with tobacco smokers and those with a history of high blood pressure.
If you are having any abnormal visual symptoms, you should always be evaluated with a thorough consultation and examination by a ophthalmologist or optometrist in NYC for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Benign Symptoms
When you develop arcus senilis or corneal arcus, the lipids in your eyes tend to concentrate in two separate parts of the corneal stroma layer: the Bowman layer and near Descemet’s membrane. On the rare occasion when it affects only one part, it’s referred to as unilateral arcus and is often found with ocular hypotony or carotid artery disease. Schnyder central crystalline dystrophy also produces arcus.
Arcus senilis is not considered a health danger or an impediment to your vision. Besides the opaque halo on the eye surface, there aren’t any other symptoms. This halo can generally be viewed without equipment, but if it’s in early or moderate development, your ophthalmologist might require the magnification instruments common in most eye care offices.
Precautions and Follow-Up
While it’s generally common that the corneal arcus is present in both eyes, it is possible for the condition to appear in just one of your eyes. In such a case, the possibility of poor ocular blood circulation could be a cause. Whenever circulation issues are suspected, your eye doctor has to investigate it.
Arcus senilis may sometimes appear as a white ring around the iris. This ring consists of calcium or lipid deposits on the circumference of the cornea, where the white section of your eye (the sclera) and the colored part (the iris) meet (called the limbus). When the deposits consist of calcium, the limbus appears milky and may indicate tissue damage that needs correction.
These white rings around the iris are considered normal with age. The “senilis” in the name is related to the word senile. Thus the condition is identified with older patients. When this white ring around the iris occurs in younger patients, however, it is generally attributed to high cholesterol levels.
The blue (or sometimes gray) ring around the iris often is associated with high cholesterol and triglycerides. In turn, this is a sign that you’re more susceptible to heart attacks and strokes. When this condition appears in people younger than 60 years old, regular blood tests are normally recommended to monitor elevated lipid levels.
Other Opaque Cornea Conditions
When your corneas become opaque, it could be from a lowered high-density lipoprotein (HDL) cholesterol level due to a genetic mutation. This condition can result in other eye problems. Principally, this opacification may be related to deficient levels of lecithin cholesterol acyl transferase (LCAT). LCAT is an enzymatic protein responsible for converting free cholesterol into cholesteryl ester.
Cholesterol ester, a hydrophobic type of cholesterol, is then separated into the nucleus of the lipoproteins to produce a synthetic high-density lipoprotein (HDL) chain. This reaction is forced one way, since the deposits are removed from the exterior. So the enzyme is attached to both HDLs and low-density lipoproteins (LDLs) in blood plasma.
This process can result in the manifestation of fish eyes, and it is actually called “fish eye disease.” Corneal opacification can also result from mutations in another HDL protein, the adenosine triphosphate-binding protein ABCA1.
If you are suffering from familial hypercholesterolaemia (FH), on the other hand, the opaqueness that’s occurring in your eyes may be emulating the excessive lipids in your blood cholesterol. You also may have what’s called lipemia retinalis, which gives a milky look to your retina. This particular manifestation of the disease seems to be aggravated by diabetes. Treatment of your diabetes and blood glucose levels can greatly enhance and improve the health of your retinas.
Diagnosis for Corneal Arcus
A diagnosis for corneal arcus can be reached through an eye exam. A trained eye doctor visually checks your eyes using an industry-approved slit lamp. A complete oral history of your family’s experience with opaqueness or other eye problems can help your ophthalmologist discover the exact nature of your condition. Corneal Arcus always be evaluated with a thorough consultation and examination by a ophthalmologist or optometrist in NYC for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Treatment for Corneal Arcus
When you have associated eye disorders, your ophthalmologist or optometrist in NYC may perform additional tests to rule out other conditions and find the cause of your eye discomfort. But since arcus senilis is considered both normal and benign for the elderly, no treatment is required or recommended.
On the other hand, arcus juvenilis is considered a danger sign for high cholesterol in younger patients. Blood tests are recommended to test for lipid and cholesterol problems. Males under the age of 40 with the condition are considered to have a higher risk for cardiovascular or coronary artery disease. Statin drugs, as well as lifestyle changes, are generally prescribed.
If you are having any abnormal symptoms, you should always be evaluated with a thorough consultation and examination by a ophthalmologist or optometrist in NYC for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Important Reminder: This information is only intended to provide guidance, not a definitive medical advice. Please consult eye doctor about your specific condition. Only a trained, experienced board certified eye doctor can determine an accurate diagnosis and proper treatment.
Do you have any questions about Corneal Arcus (Arcus Senilis) Treatment? Would you like to schedule an appointment with the best ophthalmologist in Manhattan NYC Dr. Daniel Khodadadian or optometrist, Dr. Saba Khodadadian of Manhattan Eye Doctors & Specialists? Please contact our office for a consultation with best in class eye doctors in NYC.
Dr. Saba Khodadadian, Optometrist (NYC Eye Doctor)
New York, NY 10028
(Between Madison Ave & Park Ave)
☎ (212) 533-4821


