It’s not always necessary to treat ocular hypertension, your ophthalmologist or optometrist may conclude that the risk of developing glaucoma is such that treatment is required. The most common treatment is a prescription of eye drops to alleviate the excess pressure in your eyes. There are three tests that are used to measure eye pressure: Ophthalmoscopy, Tonometry, Perimetry. Make an appointment with optometrist Dr. Saba Khodadadian and the opthamologist in NYC Dr. Daniel Khodadadian for an accurate diagnosis and treatment plan. Get the eye care you need in the safe, reassuring hands of the best rated eye doctors in NYC.
Eye Pressure (Ocular Hypertension)
 Ocular Hypertension (OHT) is a term used to describe an elevated level of intraocular pressure (IOP). More commonly, it’s the medical term for high eye pressure. Your eyeball is a spherical organ filled with two types of fluid:
Ocular Hypertension (OHT) is a term used to describe an elevated level of intraocular pressure (IOP). More commonly, it’s the medical term for high eye pressure. Your eyeball is a spherical organ filled with two types of fluid:
- The vitreous humor, a translucent gelatinous material behind the lens that fills the majority of your eyeball and maintains its shape
- The aqueous humor, a luminous fluid before the lens that fills the space between your cornea and iris
The aqueous humor is generated in and circulates through the front of your eyeball. It eventually leaks out where your cornea and iris connect. And it’s the level of this fluid that determines your eye pressure.
Think in terms of a car’s tire for an analogy. If a tire has too much air in it, the tire feels tight and stiff. Eyes are much the same in this respect. When there’s not enough pressure, they are soft and spongy, which means they’re not working at their optimal level, just like a tire. If your eye pressure is too high, however, then they’re taught and firm. While tires are measured in pounds per square inch (PSI), eyes are measured in millimeters of mercury (mmHg). Incidentally, this is same measurement for barometric pressure.
If you are having any abnormal symptoms, you should always be evaluated with a thorough consultation and examination by optometry specialist in NYC or ophthalmologist for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
What Is OHT?
“Normal” eye pressure oscillates during the day, but a general range between 10 and 21 mmHg is considered healthy intraocular pressure. Any reading above 21 mmHg may constitute ocular hypertension, as long as you don’t have optic nerve damage, visual defects, any medical reason for the elevated level, and no open angles — which refers to a type of glaucoma.
It is estimated that between four and eight percent of the American population over the age of 40 suffer from some form of OHT. Certain individuals can actually tolerate higher levels than 21 mmHg without suffering any nerve damage, while others suffer damage at lower levels. This condition is referred to as normotensive glaucoma.
Primary Causes for OHT
It’s the imbalance of the production and drainage of the aqueous humor that results in the “over-inflation” of the eye. This imbalance is necessarily a result of the lack of drainage rather than over-production. This drainage problem can be from an open or closed angle defect in your eye.
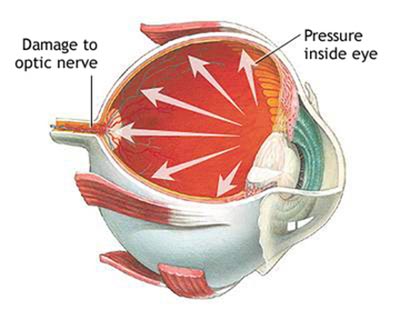
An “open angle” describes the situation where there’s a wide angle formed between your iris and cornea, but it’s somewhat clogged. Closed-angle glaucoma is where the iris inflates to close the drainage angle, thus inhibiting circulation and increasing pressure. Glaucoma occurs when the optic nerves are damaged by the excessive pressure inside the eye.
Ocular hypertension can be the result of an injury to the eye as well. In fact, it may take months or even years for the injury to result in ocular hypertension, so let your doctor know of any eye injury whenever you have an eye exam. Certain eye diseases, such as corneal arcus and pigment dispersion syndrome, are often correlated with OHT. Steroids used to treat both asthma and post-operative LASIK surgery patients are known to increase eye pressure. While the condition can afflict anyone, people with the following profiles are particularly at risk:
- Age: Eye pressure is highly correlated with increasing age, so routine testing after the age of 40 is recommended.
- Sex: Females are more likely than males to suffer from OHT.
- Race: People of African-Caribbean origin are more susceptible to ocular hypertension than those of European ancestry. Unfortunately, the condition often develops at a younger age for this demographic, so they are urged to undergo regular exams after the age of 30.
- Family history: Since it is doubtful that you’d be aware of ocular hypertension within your family, you should be cognizant of any occurrence of glaucoma in a family member and consider it a warning.
- Eyesight: If you’re suffering from severe myopia (nearsighted), you should also have your eye pressure monitored carefully.
- Cornea thickness: If you have thinner-than-average corneal measurements, you’re more likely to suffer from excessive intraocular pressure.
- Endocrine diseases: Hyperthyroidism, diabetes, acromegaly, and Cushing disease are all linked to OHT.
- Cardiovascular disease: Both coronary artery disease and atherosclerosis are associated with high eye pressure.
Pressure Behind the Eyes
The sensation of pressure behind your eyes is a symptom with several possible causes. It can be from something as simple as a tension headache. The origin of such headaches usually is the back of your neck, and from there, it stretches forward in both directions. The tension can be so severe that in addition to the pressure sensation behind your eyes, your vision can become blurry.
Graves disease is an extreme form of hyperthyroidism in which your eyes seem to bug out. This can cause a distinct pressure sensation. Glaucoma is also associated with this feeling of pressure behind your eyes, though in reality, it’s actually an intraocular pressure in the eye itself. Pressure between your eyes is generally associated with sinusitis, but you can also feel it if you suffer from migraine headaches, cluster headaches or glaucoma. if you are having any of these symptoms you should always be evaluated with a thorough consultation and examination by a optometry specialist in NYC or ophthalmologist for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Eye Pressure Test
There are three fundamental tests that are used to measure eye pressure:
- Ophthalmoscopy: Also referred to as funduscopy, this test is an examination of the back section of your eye (called the fundus), including the choroid, blood vessels, the retina, and the optic disc with a lamp designed for the purpose (ophthalmoscope).
- Tonometry: This test measures your eye pressure by gently poking your eyes with a tonometer after they’ve been numbed with eye drops.
- Perimetry: This is a visual field test to see if there are any blind spots in your peripheral vision. These spots can signal the onset of glaucoma.
How to Treat Ocular Hypertension
While it’s not always necessary to treat ocular hypertension, your ophthalmologist may conclude that the risk of developing glaucoma is such that treatment is required. In this situation, the most common treatment is a prescription of eye drops to alleviate the excess pressure in your eyes.
These medications are identical to those used to treat glaucoma itself. They function by either lowering the aqueous humour produced or increasing the drainage through the trabecular meshwork. Additionally, treating the underlying disease that’s causing the increased eye pressure helps alleviate your symptoms.
If you are having any abnormal symptoms, you should always be evaluated with a thorough consultation and examination by a optometry specialist in NYC or ophthalmologist for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Important Reminder: This information is only intended to provide guidance, not a definitive medical advice. Please consult eye doctor about your specific condition. Only a trained, experienced board certified eye doctor can determine an accurate diagnosis and proper treatment.
Do you have any questions about Eye Pressure (Ocular Hypertension)? Would you like to schedule an appointment with NY Midtown ophthalmologist or optometrist Dr. Saba Khodadadian of Manhattan Eye Doctors & Specialists? Please contact our office for consultation with NY Midtown eye doctor.
Dr. Saba Khodadadian, Optometrist (NYC Eye Doctor)
New York, NY 10028
(Between Madison Ave & Park Ave)
☎ (212) 533-4821


