Diabetic Retinopathy, Eye Disease
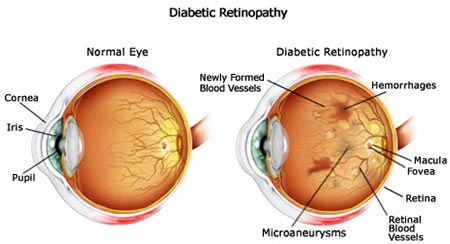 Diabetic eye disease — known by its medical term, diabetic retinopathy — is an eye issue that specifically affects people who have diabetes. If you are diabetic, you should receive specialized screenings on a regular basis. These tests are called diabetic eye exams.
Diabetic eye disease — known by its medical term, diabetic retinopathy — is an eye issue that specifically affects people who have diabetes. If you are diabetic, you should receive specialized screenings on a regular basis. These tests are called diabetic eye exams.
Diabetic eye disease affects blood vessels in your retina, which is located in the back of your eyeball. The disease is the most common cause of permanent vision loss for people who suffer with diabetes, and it’s the leading cause of blindness among adults over the age of 20.
If you are having any abnormal visual symptoms, you should always be evaluated with a thorough consultation and examination by your New York City optometrist or Dr. Daniel Khodadadian, the best eye doctor in NYC for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Related Conditions
Cataracts and glaucoma may also develop as a result of diabetic eye disease. A cataract is a hazing or clouding of the eye’s lens caused by a buildup of protein within the lens that obscures vision. Adults who have diabetes are two to five times more likely to develop cataracts than those people who don’t have diabetes. Cataracts may also form among younger-aged people with diabetes.
Glaucoma refers to a category of eye diseases that damage the optic nerve, a bundle of fibers that send and receive signals and visual information to and from your brain. Some kinds of glaucoma are linked to elevated pressure of the liquid (the vitreous) inside your eye. Glaucoma risk nearly doubles among adults who have diabetes.
Diabetic Eye Disease Causes
The cause of Diabetic Retinopathy, eye disease is a result of high blood sugar from diabetes that damages the tiny blood vessels in your retina. The function of the retina is to receive the focused light that’s projected from the lens and convert it to signals that are sent to your brain through the optic nerve.
The blood vessels that are weakened by the high sugar levels from diabetes can hemorrhage (bleed) or leak fluid, which results in distorted vision. In severe cases, the blood vessels in the retina can accumulate on the surface of the retina, which can lead to cell loss in the retina, permanent scarring and ultimately vision loss.
All types of diabetic eye disease may potentially cause permanent vision loss and blindness. Diabetic retinopathy typically progresses through four phases:
- Mild nonproliferative retinopathy: The first phase occurs when small areas of swelling called microaneurysms bloom in the blood vessels of the retina. These balloon-like areas of swelling may leak blood into your eye or fluid into your retina, obscuring your vision.
- Moderate nonproliferative retinopathy: The next phase of diabetic retinophathy occurs when the swelling blood vessels begin to distort and lose their ability to transport blood. This phase may start to change the appearance of your retina.
- Severe nonproliferative retinopathy: In this phase, the swelling, blood and fluid blocks even more blood vessels. By this point, the blood has begun to clot, preventing nutrients from reaching certain areas of your retina. These blood-deprived areas begin to secrete growths that signal the retina to grow new blood vessels to replace the blocked and damaged ones.
- Proliferative diabetic retinopathy (PDR): The final phase of diabetic retinopathy occurs when the new blood vessels formed in severe nonproliferative retinopathy become weak and fragile, at which time they also can leak and bleed. Additionally, the scar tissue from the old blood vessels that are blocked can contract and tear the retina, which causes retinal detachment, the separation of the retina from underlying tissue at the back of your eyeball. Retinal detachment may result in permanent blindness.
Symptoms of Diabetic Eye Disease
The onset of diabetic retinopathy may not present any symptoms at all. Symptoms usually only appear when the disease progresses to the state that it affects your vision. This is why it’s so important to get regular eye exams, especially if you know you have diabetes.
The blood and other fluid that leaks from blood vessels can cause eye floaters, also called blood spots in the eye. Floaters are not necessarily signs of diabetic eye disease and they can go away on their own, but without treating the issue promptly, you increase the risk of permanent vision loss. If you are having any visual abnormalitoes you should always be evaluated with a thorough consultation and examination by a ophthalmologists NYC for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Diagnosis and Detection of Diabetic Eye Disease
Diabetic retinopathy and diabetic macular edema (DME) may both be detected through a comprehensive dilated eye exam. Diabetic macular edema is a similar leaking of fluid from blood vessels created by diabetes, but is more focused in the macula — the part of the retina that deals with detailed vision. DME is only formed after diabetic retinopathy is present.
The dilated eye exam includes the following procedures:
- Visual acuity testing: This is an eye chart test that determines your ability to see at various distances.
- Pupil dilation: Your pupil is dilated (widened) with drops placed on the surface of your eye. This allows your eye care professional to examine the optic nerve and retina inside your eye.
- Tonometry: This painless test measures the pressure inside your eyeball.
- Optical coherence tomography (OCT): The OCT test is like an ultrasound, but uses light waves instead of sound waves to detect tissues inside your body. An OCT test provides detailed images inside your eye that can be penetrated by light.
Treatment for Diabetic Retinopathy, Eye Disease
Vision lost to diabetic eye disease may sometimes be irreversible. However, early detection and treatment can decrease the risk of permanent blindness by 95 percent. Diabetic eye disease may often lack symptoms, so if you have diabetes, you should receive comprehensive diabetic eye exams at least once a year.
Those people who test positive for diabetic retinopathy may require eye exams more frequently than once per year. It’s important that women who are pregnant and have diabetes receive a diabetic eye exam as soon as possible. Exams throughout the pregnancy may be required as well.
According to a study by the Diabetes Control and Complications Trial (DCCT), when people control their diabetes, it slows the worsening of diabetic retinopathy. The study participants who kept glucose levels close to normal were significantly less likely than those who had higher glucose levels to develop diabetic retinopathy — in addition to nerve and kidney diseases. Other trials by the DCCT have demonstrated that controlling elevated cholesterol and blood pressure decreases the chance of vision loss among people with diabetes.
Once DME develops from diabetic eye disease, your ophthalmologist can treat it with Anti-VEGF Injection Therapy. Anti-VEGF medications are injected into the vitreous to block a protein that stimulates irregular blood vessels to grow and leak blood or fluid.
If you are having any abnormal visual symptoms, you should always be evaluated with a thorough consultation and examination by a physician for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Important Reminder: This information is only intended to provide guidance, not a definitive medical advice. Please consult eye doctor about your specific condition. Only a trained, experienced board certified eye doctor can determine an accurate diagnosis and proper treatment.
Do you have any questions about Diabetic Retinopathy, Eye Disease? Would like to schedule an appointment with leading Ophthalmology, retina specialist in NYC or Optometrist, Dr. Saba Khodadadian Manhattan Eye Specialists, please contact our office for consultation with New York City Eye specialist.
Dr. Saba Khodadadian, Optometrist (NYC Eye Doctor)
New York, NY 10028
(Between Madison Ave & Park Ave)
☎ (212) 533-4821


