Tear gland inflammation treatments are geared to your specific problem since there are such an assorted variety of potential causes. In most cases, tear gland inflammation can be treated with the use of oral antibiotics prescribed by your NYC eye doctor. If you don’t begin to show major improvement in the first couple days, surgery may be necessary. In the chronic cases a newer treatment methods include soft contacts infused with artificial tears and time-released medications. Make your appointment with the best in class eye doctors in NYC, meet our New York optometrist Dr. Saba Khodadadian and ophthalmologist Dr. Richard L. Deluca.
Tear Gland Inflammation
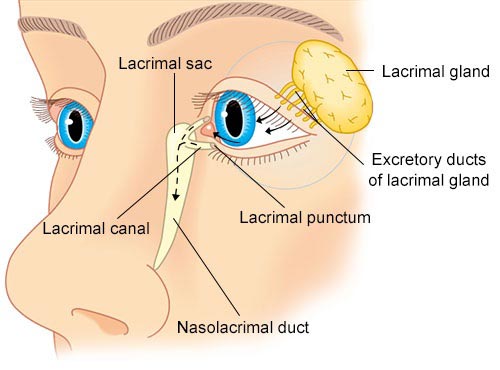 Your eyes produce tears to stay lubricated for comfort and free from dust, particles or debris. However, if your tear glands become swollen or inflamed for any reason, it can be an extremely unpleasant experience.
Your eyes produce tears to stay lubricated for comfort and free from dust, particles or debris. However, if your tear glands become swollen or inflamed for any reason, it can be an extremely unpleasant experience.
The glands that produce tears are called the lacrimal glands, but are more commonly known as the tear ducts. The medical term for the condition that causes inflammation in your tear ducts is dacryoadenitis. This may occur in one or both eyes, and the condition can be either chronic or acute, meaning it can present as a temporary problem or an ongoing issue.
If you are having any abnormal symptoms, you should always be evaluated with a thorough consultation and examination by a ophthalmologist or New York optometrist for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Symptoms to Expect
When your tear glands become inflamed, it’s likely to be first noticed as an increasing redness and discomfort. The outside surrounding eye lid can become quite swollen and painful to the touch. There may be a sensation of pressure as the swelling increases.
Dry or watery eyes both can be symptoms, depending on whether the swelling is blocking the duct or pushing out excess tears. The inflammation also can produce a sticky discharge that forms a crust on your lashes. Some more severe cases may even include fever or upper respiratory infection.
Causes Can Vary
The acute (but temporary) cases of tear gland inflammation are generally the result of a viral or bacterial infection. Fungal infections are also possible, but are actually quite rare. The most common are:
- Viral
- Mumps
- Cytomegalovirus
- Echoviruses
- Epstein-Bar virus
- Herpes Zoster (shingles)
- Mononucleosis
- Coxsackievirus A
- Bacterial
- Staphylococcus
- Streptococcus
- Gonorrhoeae
- Chlamydia
- Tuberculosis
- Fungal (rare)
- Parasite
- Histoplasmosis
- Protozoa
- Blastomycosis
The ongoing chronic cases are usually caused by swelling and inflammation issues that aren’t related to infection. Thyroid eye disease is a common source of trouble for the lacrimal glands. Sometimes, pseudotumors occur. These tumors are called “pseudo” because they’re inflamed growths or masses that only resemble tumors. They are, in fact, not cancerous. Sarcoidosis, formations of inflammatory cells, may also be the problem. If you are having any of these symptoms you should always be evaluated with a thorough consultation and examination by a ophthalmologist or New York optometrist for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Common Occurrences
Blocked tear ducts most often happen in babies, although they can still happen, no matter how old you are. One in three babies is affected by tear gland inflammation. It causes excessive tearing, redness, and discharge when there’s no other apparent sickness problems or allergies. Lots of babies are born with a thin piece of skin, like a membrane that doesn’t allow the duct to open properly or makes it too narrow for the passage of tears. This can require a minor 5-to-10-minute procedure to correct.
Infection in adults usually begins as a response to a tear duct blocked by the way your bones grow. This can make your tear ducts a lot narrower than they should be.
Accurate Diagnosis Required
To diagnosis tear gland or duct inflammation, you’ll need to undergo a thorough examination of your eyes and eyelids because there may potentially be a very serious problem. Biopsies, CT scans and other special tests may be necessary to check for tumors.
A blocked tear duct can result from several issues, including:
- Thin tissue at the end of the tear duct doesn’t open right, causing it to get infected
- Bone growth of your nose bone can restrict the tear duct and cause pressure
- Several types of infection
- Your eyes may even have underdeveloped openings where your tears meet your ducts
Potential Symptoms
Tear gland inflammation runs in families, or it can be the result of injury. If you have a blocked tear duct, several things could happen:
- You may experience wet and watery eyes. You may even have tears rolling down your face at times.
- A white or yellow discharge could build up in your eye.
- Possible swelling may occur around your eye and nose.
The swelling around your eye and nose area could possibly indicate an infection in your eye’s drainage system. This is what’s either caused by or causes the tear glands to get inflamed.
Lacrimal Apparatus
The lacrimal apparatus is your body’s system of producing and draining tears, a delicate and precise process. The slightest infection, defect or difference can upset the entire give-and-take balance. This can even happen from shifts in hormone levels. These hormonal issues present most commonly in women when they become pregnant or go through menopause.
Dry eye is one of the conditions that can result from lacrimal apparatus disorders and is likely the one most seen by ophthalmologists. Disorders of the lacrimal apparatus are often affected by environmental factors such as weather and smoking because these types of outside factors can rob your eyes of much needed moisture. Reading or staring at computer screens also can make your symptoms worse because you tend to blink less frequently during these activities.
Treatment of Tear Gland Inflammation
Treatments are geared to your specific problem since there are such an assorted variety of potential causes. In most cases, tear gland inflammation can be treated with the use of oral antibiotics prescribed by your NYC eye doctor. These usually work quite quickly and can actually clear up the infection in a couple days while your overall discomfort improves nearly overnight. If you don’t begin to show major improvement in the first couple days, surgery may be necessary to clear the tear duct itself, or any bone or growths that may be restricting the tear duct in any way.
In the chronic cases, treatment proves to be continuous in an effort to manage your symptoms. Eye drops and ointments become a staple item in your medicine cabinet. However, treatment of eye conditions is progressing along with the rest of technology. Some newer treatment methods for ocular disorders include soft contacts infused with artificial tears and time-released medications that go under your lower eyelid.
Possible Complications
The worst case scenarios involve malignancies in the tear duct or such severe swelling that that it puts enough pressure on your eye to affect your vision. To prevent future problems, it’s advisable to keep your vaccinations up to date. Drinking plenty of water and maintaining a healthy diet can also keep your overall inflammation to a minimum.
If you are having any abnormal visual symptoms, you should always be evaluated with a thorough consultation and examination by a ophthalmologist or New York optometrist for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Important Reminder: This information is only intended to provide guidance, not a definitive medical advice. Please consult eye doctor about your specific condition. Only a trained, experienced board certified eye doctor can determine an accurate diagnosis and proper treatment.
Do you have any questions about Tear Gland Inflammation treatment in NYC? Would you like to schedule an appointment with the top ophthalmology specialist Dr. Richard L. Deluca and a top rated optometrist Dr. Saba Khodadadian of Manhattan Eye Doctors & Specialists? Please contact our office for consultation with the best rated New York eye doctors.
Dr. Saba Khodadadian, Optometrist (NYC Eye Doctor)
New York, NY 10028
(Between Madison Ave & Park Ave)
☎ (212) 533-4821


