The specific eye inflammation treatment depends on the type of uveitis that you present. Some treatments — like corticosteroid eye drops — exclusively target an eye, while other forms of treatment — such as immunosuppressive agents — are ingested in pill form when the affliction affects both eyes. For autoimmune issues, your eye doctor may prescribe medications such as cyclosporine, azathioprine, mycophenolate or methotrexate. Contact your ophthalmologist Dr. Daniel Khodadadian in NYC if you experience eye inflammation (Uveitis). Get the eye care you need in the safe, reassuring hands of the best rated NYC opthamologist.
Eye Inflammation (Uveitis)
 Uveitis, or eye inflammation, is a broad term that describes several inflammatory diseases that produce swelling in the eyes and can destroy eye tissue. These diseases also degrade your vision and can lead to severe loss of vision.
Uveitis, or eye inflammation, is a broad term that describes several inflammatory diseases that produce swelling in the eyes and can destroy eye tissue. These diseases also degrade your vision and can lead to severe loss of vision.
Eye inflammation typically occurs in a part of the eye called the uvea (hence the name uveitis), but it’s not limited to that area. These inflammation diseases may also affect the retina, lens, vitreous and optic nerve, resulting in reduced vision and even permanent blindness. Your eye care professional may refer to uveitis more specifically as anterior uveitis, posterior uveitis, intermediate uveitis, or panuveitis. It may also be described as infectious or noninfectious.
At Manhattan Eye Doctors & Specialists, Dr. Khodadadian, a top rated optometrist in New York City, optometry specialist and Dr. Daniel Khodadadian, an opthamologist in NYC offers varying eye care treatments from simple vision test to the most complex eye surgeries.
Uveitis may stem from eye diseases, or it can be the result of an inflammatory disease that affects other areas of the body as well. Uveitis affects people of all ages, but primarily impacts people between the ages of 20 and 60. Eye inflammation can be acute (lasting a short time) or chronic (with a long duration). Uveitis can clear up and reappear many times.
If you are having any abnormal visual symptoms, you should always be evaluated with a thorough consultation and examination by a physician for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Causes of Eye Inflammation
The body’s natural reaction to germs, toxins and tissue damage is inflammation. Uveitis generally is caused by inflammation that develops in your eye. Inflammation produces redness, heat and swelling, and it destroys tissues as a result of white blood cells flooding the affected area to eliminate the contamination.
Uveitis typically is caused by:
- Infections, growths or tumors growing in your eye or in other regions of your body
- Autoimmunity issues (in which your body’s own immune system attacks itself)
- Toxins that have penetrated your eye
- Eye bruises
Types of Eye Inflammation
Uveitis is classified by the location in the eye where it occurs. The different types of uveitis, therefore, affect different parts of your eyes. The most severe forms of uveitis are intermediate, posterior, and panuveitis. If left untreated, these conditions can cause blindness.
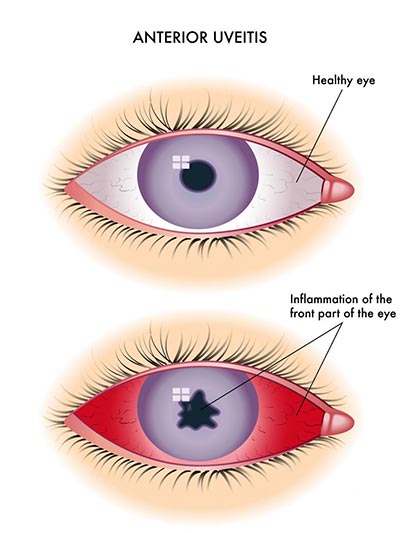
- Anterior Uveitis: Anterior uveitis is inflammation in the front of your eye. It’s the most common form of eye inflammation and typically occurs in young and middle-aged people. Most anterior uveitis cases only affect one eye, and it usually occurs in otherwise healthy people.
- Intermediate Uveitis: Intermediate uveitis occurs in the fluid of your eye (called the vitreous). It’s most common in young adults and has been linked to disorders such as multiple sclerosis and sarcoidosis.
- Posterior Uveitis: Posterior uveitis occurs in the back of your eye — in the retina and the choroid. It’s the least common type of eye inflammation. This condition is also known as choroditis or chorioretinitis. Many infectious and non-infectious conditions cause posterior uveitis.
- Panuveitis: Panuveitis is the term for inflammation occurring in all three major parts of the eye. The most common disease causing panuveitis is Becket’s disease, which leads to severe damage to your retina.
Symptoms of Eye Inflammation
Uveitis or eye inflammation has many sources, but often the exact cause is unknown. Uveitis can affect one or both eyes. The various forms of uveitis may present different types of signs and symptoms. The symptoms typically include:
- Eye pain
- Redness of the eye
- Decreased vision
- Increased eye floaters
- Light sensitivity
Acute anterior uveitis is characterized by blurred vision, eye pain, small pupil, redness and sensitivity to light. With intermediate uveitis, you’re more likely to get symptoms that include floaters and blurred vision, with little or no pain. Posterior uveitis, if left untreated, creates vision loss. This form of uveitis can only be detected by an vision exam. If you are suffering severe forms of these symptoms — especially eye pain, change in vision or extreme light sensitivity — see an ophthalmologist as soon as possible for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Diagnosis of Eye Inflammation
The diagnosis of eye inflammation involves a thorough exam by an eye care professional, including a study of your full medical history. Lab tests may be ordered to rule out autoimmune issues or infection. If you have intermediate uveitis, a central nervous system examination may be conducted to rule out multiple sclerosis.
The typical eye exams that are conducted to detect and diagnose uveitis include:
- Eye chart or visual acuity test
- Funduscopic exam
- Ocular pressure exam
- Slit lamp exam
Eye Inflammation, Uveitis Treatment
An ophthalmologist generally prescribes anti-inflammatory medicine that can be taken as a pill, used as eye drops, injected into the eye, taken intravenously, or released from a capsule that is surgically implanted into your eye. Uveitis treatments typically aim to:
- Reduce inflammation
- Prevent further damage to tissues
- Alleviate pain
- Restore vision loss
The specific treatment depends on the type of uveitis that you present. Some treatments — like corticosteroid eye drops — exclusively target an eye, while other forms of treatment — such as immunosuppressive agents — are ingested in pill form when the affliction affects both eyes. For autoimmune issues, your eye doctor may prescribe medications such as cyclosporine, azathioprine, mycophenolate or methotrexate. Each of these medicines requires frequent blood tests to monitor potential side effects.
Anterior uveitis commonly is treated by eye drops to dilate your pupil and prevent muscle spasms, followed by eye drops containing steroids to reduce inflammation. Intermediate, posterior, and panuveitis require more advanced uveitis treatments like injections around the eye or the surgically implanted capsules.
Safety and Effectiveness of New Uveitis Treatments
A National Eye Institute (NEI) study, known as the Multicenter Uveitis Steroid Treatment (MUST) Trial, compared the effectiveness and safety of the treatments that suppress your immune system with a new uveitis treatment that only focuses on the immune system in your eyes. The first group of patients were given high doses of prednisone for one to four weeks, and then gradually reduced. The second group involved capsules that released another corticosteroid called fluocinolone. These capsules were surgically implanted in the eyes. The result of the study is that both treatments improved vision to a comparable degree.
The patients in the first group that received the conventional treatment had few side effects, whereas the surgical implant group showed more side effects and eye problems, such as glaucoma, cataracts and high eye pressure. Both treatments were effective in decreasing inflammation, but the implant was much faster at reducing it and reduced it to a greater degree. Overall, the visual improvements in both groups of patients were similar to one another.
If you are having any abnormal symptoms, you should always be evaluated with a thorough consultation and examination by a physician for an accurate diagnosis and treatment plan as it may be a symptom or sign of a serious illness or condition.
Important Reminder: This information is only intended to provide guidance, not a definitive medical advice. Please consult eye doctor about your specific condition. Only a trained, experienced board certified eye doctor can determine an accurate diagnosis and proper treatment.
Do you have any questions about Eye Inflammation (Uveitis) Treatment? Would like to schedule an appointment with New York City’s leading Ophthalmologist Dr. Daniel Khodadadian or New York optometrist Dr. Saba Khodadadian of Manhattan Eye Doctors & Specialists, please contact our office for consultation with NYC Eye doctor.
Dr. Saba Khodadadian, Optometrist (NYC Eye Doctor)
New York, NY 10028
(Between Madison Ave & Park Ave)
☎ (212) 533-4821


